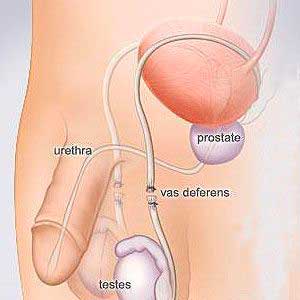
Vasectomy
Vasectomy involves closure of the vas deferens, the conducts allowing spermatozoa to pass from the testicle to the outside.
The vas deferens is located close to the vessels of the spermatic cord and can easily be identified from the outside as a small cord close to the testicular vessels.
Vasectomy represents the safest, simplest and most effective form of permanent contraception. It involves a small incision to the scrotum under local anesthetic, a few hours’ recovery and quick return to normal activities. It does not cause side effects. Vasectomy is a safe procedure with an extremely low level of complications: specifically, testicular function is preserved and the production of sex hormones remains unchanged as does spermatogenesis within the testicle. Minor complications after the procedure include complications common to any surgical procedure such as hematoma or wound infection, but these are easily controlled with appropriate local disinfection and the application of an ice pack. One rare complication (0.4-5%) is chronic epididymal pain. As well documented in various studies, complications also depend on the surgeon’s experience.
The no-scalpel vasectomy is an even less invasive procedure carried out via a single central incision rather than via two small bilateral incisions. Initially, it is carried out under local anesthetic.
The vas deferens is palpated and isolated using a specific instrument with a ring. It is then sectioned and the two ends are tied. The same procedure is then carried out for the contralateral vas deferens. At the end of the procedure, the scrotal incision is barely visible.
This kind of technique is the quickest and keeps post-operative symptoms, hemorrhages and infections to a minimum.
- the vasectomy procedure is considered definitive
- the possibility of cryo-preserving spermatozoa is considered in case the patient changes his mind in the future
- the choice to undergo vasectomy can be shared within a couple, although the final decision is, naturally, the man’s
- it is possible to micro-surgically re-canalize the vas deference via a reversal technique, although this does not guarantee restoration of natural fertility
How long after the vasectomy do you become sterile?
Directly after the vasectomy procedure, in the seminal tubules and particularly in the seminal vesicles, large quantities of spermatozoa are present, which need to be expelled before the man becomes sterile. It is estimated that it will take around 15 ejaculations in order to eliminate these spermatozoa. In any case, it is necessary to have 2 sperm analyses showing the absence of spermatozoa before being considered sterile.